Science and ethics
For many in the modern Western world the transition from life to death has become a question of science.
The ‘medicalisation’ of death and dying has led to it being seen as a problem to be dealt with by professionals and removed from everyday life.
What are the ethics, the rights and wrongs, of this approach? Do we want death to be part of our lives, to embrace the dying and their wishes?
Or are we happy to think about it only when we have to?
Prolonging life
How far should we go to extend human life?
Green glass box in the shape of a peach, China late 18th century
 According to Chinese folklore, eating the Peaches of Immortality can grant ever-lasting life to humans. In Chinese art the peach represents the wish for a long and healthy life.
According to Chinese folklore, eating the Peaches of Immortality can grant ever-lasting life to humans. In Chinese art the peach represents the wish for a long and healthy life. Medicine chest for use in the home, England early 19th century
 Until the mid-1800’s the practice of medicine was unregulated so many people kept their own natural remedies for the treatment of minor wounds or as painkillers or purgatives (inducing vomiting or sweating).
Until the mid-1800’s the practice of medicine was unregulated so many people kept their own natural remedies for the treatment of minor wounds or as painkillers or purgatives (inducing vomiting or sweating).For tens of thousands of years most societies have been using plants for medicinal purposes. Between 4,000 and 2,000 years ago the Ancient Egyptians, Babylonians and Greeks improved treatments and surgery based on observations of how the body worked. By the 20th century in Europe and the rise of modern medicine, great advancements in the attempt to preserve and extend human life had been achieved.
The first human organ transplant was a kidney transplant performed in 1954 in the USA. Today in the UK there are over 7,000 people on the transplant waiting list. A few hundred people, in another attempt to challenge the boundaries of human life, have chosen to be frozen after their deaths. Their bodies wait in suspension until science has advanced to the point that they can be resuscitated and cured of whatever killed them.
“The right to die can easily become the duty to die.”
Caring for the dying
When do you start to die?
Graseby MS 26 Portable Daily Rate Syringe Driver MS26
 Syringe drivers can be used to help control pain. They work by delivering a steady flow of injected medication continuously under the skin.
Syringe drivers can be used to help control pain. They work by delivering a steady flow of injected medication continuously under the skin.Oral healthcare pack
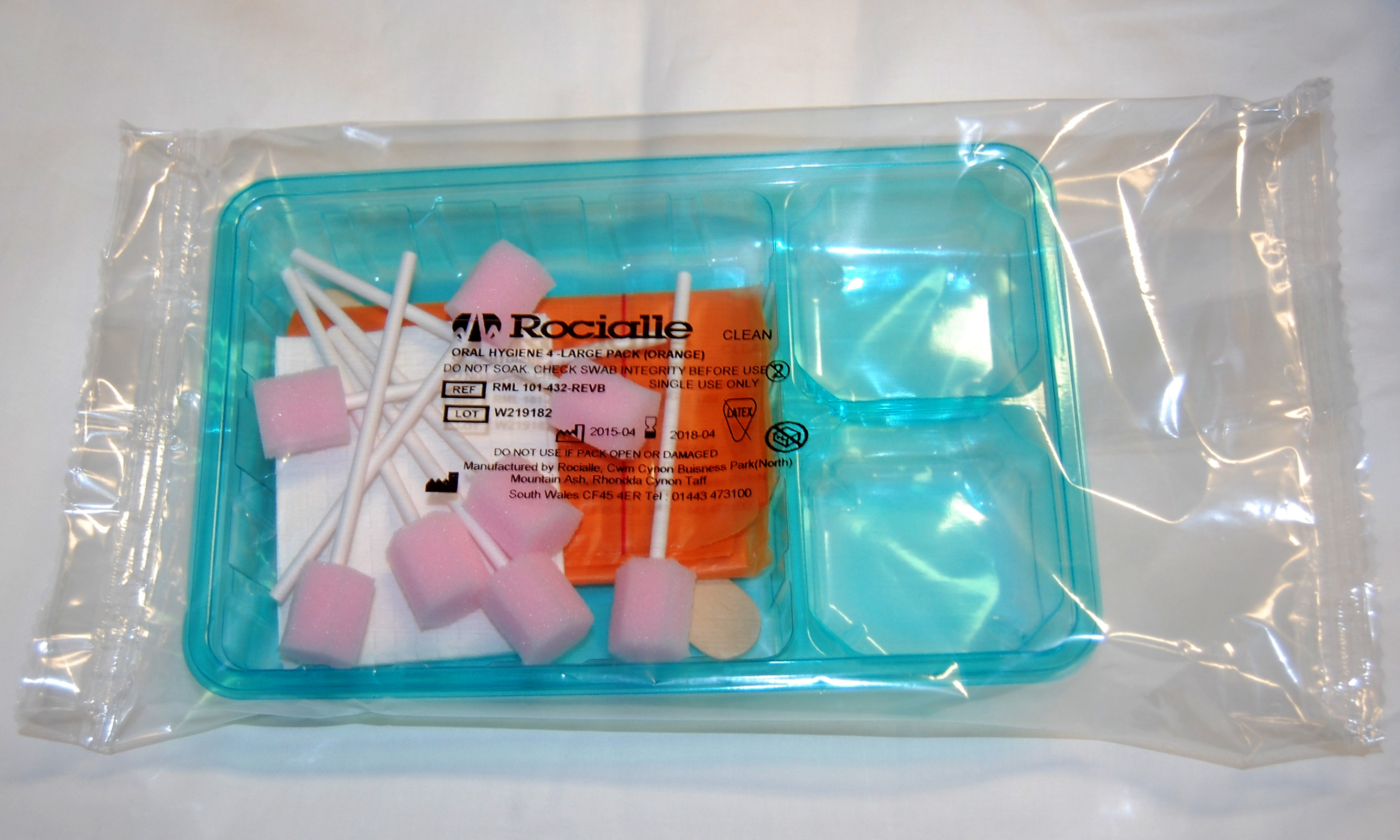 This pack contains swabs that are used to clean and hydrate the mouths of people at the end of their lives when it is difficult for them to do so for themselves.
This pack contains swabs that are used to clean and hydrate the mouths of people at the end of their lives when it is difficult for them to do so for themselves.For some people death is sudden and unexpected. For some it is a gradual decline into old age. For others, the start of the dying process can be said to begin with a diagnosis of a life-limiting illness, where death will be a direct consequence. Some medical professionals regard the start of the dying process as being within 12 months of the end of life or when it is imminent, only a matter of days or hours away.
As the illness progresses and your body begins to stop working medical intervention, known as life-sustaining treatment, can be offered to temporarily stabilise the body. The period from diagnosis to death can last for several years. During this time a range of healthcare services, known as palliative care, is made available to you and your family. These services can include pain management strategies and psychological and emotional support.
“I believe it is a fundamental human right for every adult of sound mind, to be able to plan for the end of their life in a way that is reliable, peaceful & at a time of their choosing.”
End of life choices
Whose death is it?
Medication
 Two empty medication bottles used by the not-for-profit members society Dignitas in ‘accompanied suicides’ in Switzerland – Paspertin is an anti-nausea medicine given before a lethal dose of pentobarbital. Each dose of pentobarbital is prescribed by a registered Swiss doctor for a specific patient. Chocolates are eaten directly after the last dose to mask the bitter taste of the medication.
Two empty medication bottles used by the not-for-profit members society Dignitas in ‘accompanied suicides’ in Switzerland – Paspertin is an anti-nausea medicine given before a lethal dose of pentobarbital. Each dose of pentobarbital is prescribed by a registered Swiss doctor for a specific patient. Chocolates are eaten directly after the last dose to mask the bitter taste of the medication.Until the mid-20th century most people died at home with their family and community around them. We now live longer into old age and most people die in hospitals, hospices or care homes with a large variety of professionals involved in our deaths. However, there are various ways you can make choices in the way you die.
You can refuse life-sustaining treatments at the time they are offered. You can complete in advance a document outlining what you do or do not want to happen, such as a do-not-resuscitate order, in case later you are unable to communicate. What is not available legally in the UK is euthanasia or assisted dying. Healthcare professionals can not intentionally end life even to relieve suffering or to help someone who wants to die achieve this. Assisted dying is legal in Switzerland, the Netherlands, Belgium, Luxembourg, Germany and several states in the USA.
death: is it your right to choose?
Our second death related exhibition, death: is it your right to choose? looked at end-of-life options in this country and focused on whether we should allow assisted dying to be legalised.
We chose to use a re-creation of a room at the Dignitas flat near Zurich as a thought-provoking starting point for this discussion.
After seeing the exhibition, we asked visitors if they thought the law in this country should allow assisted dying. The below chart shows the results of this question in the survey: